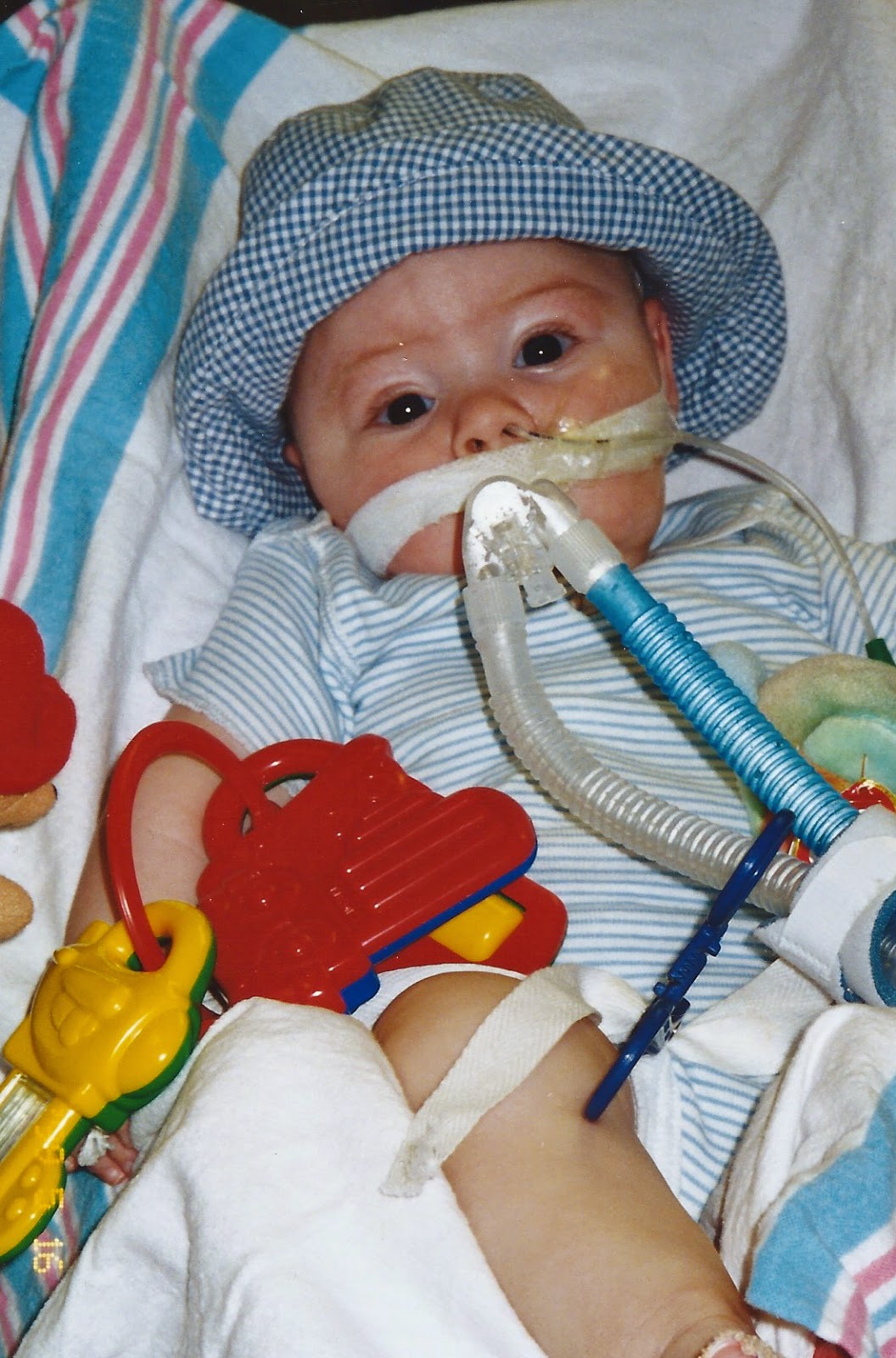
As I sit here,
the night before I leave to spend a week in St. Louis – the City where Jack’s
journey began, I think of where we were fifteen years ago at this same
time. Jack was in the Pediatric
Intensive Care Unit at St. Louis Children’s Hospital (SLCH) recovering from
surgery three days prior to plicate his right diaphragm in an attempt to
resolve the persistent collapse of his right lung that was thought to be the
cause of his inability to successfully wean from the hospital ventilator.
Thinking of those
early memories and realizing that I only started blogging in 2006, when Jack
was 8 years old, I decided that I need to go back in time and document the
first eight years of Jack’s life as best as I can remember, before I forget it
all. I titled this entry Part II
because it details Jack’s admission to the Pediatric Intensive Care Unit at St.
Louis Children’s Hospital in January of 1999. I’m starting with Jack’s time in
the PICU at St. Louis Children’s because that’s where my memories are right now
as I anticipate my upcoming visit to St. Louis. I’ll write Part I at a later time.
JACK’S JOURNEY –
THE EARLY YEARS, PART II
Jack was
discharged from the Special Care Nursery at Missouri Baptist Medical Center on December
22, 1998, a little more than six weeks after he was born. Jack required a small amount of oxygen
to keep his O2 saturations at an acceptable level. At the time, I thought lugging around
an oxygen tank in the freezing cold and snow was the biggest inconvenience of
my life. (Ha!)
Once home, Jack
appeared to be doing well, although he struggled to coordinate eating with
breathing, which made feeding time very stressful for all parties involved. One
night, sometime during the second week in January – I don’t remember the exact
day, Jack, who at that time was able to easily move his arms and legs, was kicking so much that he kept setting off his pulse-ox because it couldn’t pick up his
numbers. I was on “Jack duty” that night, which meant I was sleeping on the
couch in the family room next to Jack’s basinette. I was so tired because I wasn’t getting much sleep caring for a
newborn who struggled to eat. After being awakened more times than I could
count for false alarms triggered by Jack’s constant movement, I was so
desperate for sleep that I took the pulse-ox off of Jack’s foot. (Clearly, this was before I appreciated the importance of a pulse-ox.) After falling back to sleep, I was
startled awake by a sound that I didn’t recognize but, for reasons I attribute
solely to the grace of God, motivated me to get up and check on Jack. When I looked into Jack’s crib he
wasn’t moving and his color was ashen. I picked him up and he was as limp as a ragdoll. Everything I had been taught about CPR
before leaving the Special Care Nursery with Jack was lost in my state of
absolute panic. I ran over to the stairs with Jack in my arms and screamed for
Mark. Mark came running down the
stairs, grabbed Jack out of my arms and proceeded to give Jack rescue breaths,
which did indeed rescue him. I think it’s fair to say that I came a long way
from that day when dealing with Jack’s future episodes of respiratory
distress. I also think it's fair to say that had I not woke up when I did, Jack's journey would have ended that day.
Jack’s apneic event
bought him an ambulance ride to Missouri Baptist Medical Center. From there,
Jack was transported via a mobile ICU to St. Louis Children’s Hospital, where
he was admitted to the Pediatric Intensive Care Unit. This was my very first
experience with an intensive care unit and to say I was shell-shocked is an
understatement. The lights were bright, there were multitudes of medical people milling around in a
very small space, and alarms were going off non-stop all around me. I was
overwhelmed and completely lost.
They put Jack on
nasal CPAP because his end tidal CO2 was 120 (normal is 35-45). I was a mess
because I did not like seeing Jack hooked up to any type of breathing
assistance. Little did I know what awaited us. While in the PICU, they discovered that Jack was born with an aortic anomaly called a vascular ring. Jack’s aorta arched
to the right (normal is to the left) forming a ring with his anomalous left
subclavian artery. The vascular
ring was compressing Jack’s trachea and esophagus - an explanation for Jack’s
difficulty with eating and breathing. On January 18, 1999, Jack had surgery to divide the vascular ring. I was terrified to see Jack after surgery knowing that his chest had been cut open and his sternum sawed apart. I remember slowly walking to Jack's bed after surgery, almost with my eyes closed, peeking just enough to take it all in a little bit at a time. Standing at Jack's bedside, I felt like I was going to throw up. He had so many tubes coming out of his tiny 5-pound body.
post-op vascular ring division
Following surgery, Jack had a hard time coming off the hospital ventilator. They extubated him shortly after surgery, but he had to be reintubated and it was ten days post-op before he was able to wean from the ventilator. Jack was discharged approximately two weeks after surgery. When we walked out of the hospital with Jack, I thought the problem had been found and resolved and that Jack was on the road to recovery and a normal life.
I was so wrong.
finally off the ventilator post-op
Within two days
of coming home, we had to bring Jack back to the emergency department at St.
Louis Children’s because he was in respiratory distress again. An X-ray showed that Jack had a
partially collapsed right lung. Jack was admitted to the PICU again and was placed
back on nasal CPAP again. He eventually transferred to the floor, where he
spent another two weeks while they weaned him off CPAP during the daytime
hours. It was also discovered during this admission that Jack had an elevated
right diaphragm, which was determined to be the result of damage to the phrenic
nerve during the surgery to divide the vascular ring. Damage to the phrenic nerve is a known risk of cardiac
surgery. Just one of the many breaks Jack never got.




After three weeks
in the hospital, Jack came home on nasal CPAP and supplemental oxygen. But our
reprieve was short-lived. Two weeks after being discharged from SLCH the second
time, Jack landed back in the PICU because he was in respiratory distress yet
again. On March 7, 1999, Jack was intubated
and placed on the ventilator. Jack never again breathed without the assistance
of a ventilator.
One week after
being admitted, the first attempt was made to extubate Jack from the
ventilator. Jack didn’t last more than a few hours. After Jack failed extubation, the decision was made to
perform surgery to plicate Jack’s right diaphragm in an attempt to resolve the
right lung collapse that was believed to be the cause of Jack’s episodes of
respiratory distress.
Following
surgery on March 30, 1999, another attempt was made to remove Jack from the
ventilator. Again, Jack failed
extubation. At this point, the
PICU team asked for neurology to consult because they felt that Jack
demonstrated low tone and muscle weakness. They didn’t know if Jack’s weakness was due to his
prematurity and all the surgeries he had been through or due to an underlying
disease.
resting post-op diaphragm plication

As a side note, this was the beginning
of me making waves when it came to Jack and his care. In Jack's early PICU days, I wasn't yet tuned in to hospital
politics and knowing who does what and, more importantly, who doesn't do what. Being
the naive person I was, when I heard neurology wanted a muscle biopsy, I
decided right then and there that I wanted Jack’s cardiothoracic surgeon to do
the procedure because he had already cut on Jack twice and I trusted him. Plus, he adored Jack. The PICU staff seemed a bit
uncomfortable with my request, but they honored it and forwarded my request on
to Jack’s CT surgeon. The surgeon was kind enough to do Jack's muscle biopsy
(bedside in the PICU). I say "kind enough" because, typically,
cardiothoracic surgeons don't do muscle biopsies. They have more important
surgeries on their schedules - like heart and lung transplants. In retrospect,
I vaguely remember the surgeon not really being that happy about doing the
muscle biopsy. (You could see and hear a lot more of what was going on in the
PICU back in those days because the PICU rooms were pods separated only by curtains,
which were usually open.) But, when he came over to Jack's bed to talk with me,
he said "yes" he would be happy to do the muscle biopsy. He really
wasn't!
But, I digress.
The preliminary results of the muscle
biopsy suggested an inflammatory myopathy. Jack was started on high dose
steroids and, after several weeks on the steroids, another attempt was made to
extubate Jack. Again, Jack failed.
on high dose steroids and miserable
last failed attempt at extubation before trach
I first heard the word “tracheostomy”
following Jack’s first failed attempt at extubation. I didn’t know much about a
trach – I had never seen one, but one thing I did know was that I wanted nothing
to do with it. I was adamant that I wasn’t going to consent to a trach until
the doctors could tell me exactly why Jack needed one. I needed a diagnosis. In
desperation, every time they attempted to remove Jack from the ventilator, I’d
leave the PICU and go to the hospital chapel where I’d spend hours saying the
rosary and begging God, Mary (the mother of God) and anyone else “up there” who
might be listening, to please let Jack breathe on his own without the
ventilator. My prayers went
unanswered.
After multiple failed attempts at
extubation and with all options considered and tried, ten weeks after Jack was
first intubated, I finally relented.
I signed the consent form for Jack to get a tracheostomy, despite having
no diagnosis or prognosis.